what is ttp, check these out | What is TTP and how do you get it?
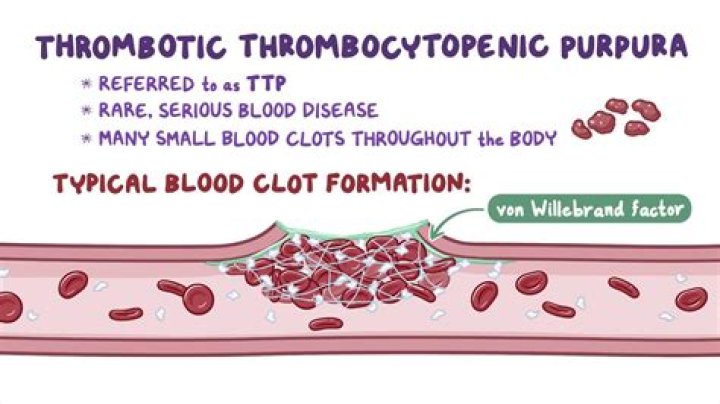
Thrombotic thrombocytopenic purpura (TTP) is a blood disorder in which platelet clumps form in small blood vessels. This leads to a low platelet count (thrombocytopenia).
What is TTP and how do you get it?
A lack of activity in the ADAMTS13 enzyme (a type of protein in the blood) causes thrombotic thrombocytopenic purpura (TTP). The ADAMTS13 gene controls the enzyme, which is involved in blood clotting. Not having enough enzyme activity causes overactive blood clotting.
Can TTP be cured?
Can TTP Be Cured? About 80% of patients will survive. The majority of patients will have only one episode of TTP; few will have relapses.
What drugs cause TTP?
In this review, five drugs that have been the subject of the most and the most recent reports of drug-associated TTP-HUS are discussed: mitomycin C, cyclosporine, quinine, ticlopidine, and clopidogrel.
How long can you live with TTP?
The most striking evidence for the impact of morbidities following recovery from TTP is decreased survival. Among the 77 patients who survived their initial episode of TTP (1995-2017), 16 (21%) have subsequently died, all before their expected age of death (median difference, 22 years; range 4-55 years).
What are signs and symptoms of TTP?
Symptoms
Bleeding into the skin or mucus membranes.Confusion.Fatigue, weakness.Fever.Headache.Pale skin color or yellowish skin color.Shortness of breath.Fast heart rate (over 100 beats per minute)
What should be avoided during TTP?
Do not drink or eat anything that contains quinine.
Quinine can make TTP worse. Quinine is found in tonic water, flavored drinks, and some foods. Read all food and drink labels to check for quinine. Ask your healthcare provider for a full list of drinks and foods that contain quinine.
Is TTP painful?
Abdominal pain is frequently encountered in patients with thrombotic thrombocytopenic purpura (TTP). Often the pain is secondary to inflammation of the pancreas.
Is TTP inherited?
Congenital TTP is caused by changes ( mutations ) in the ADAMTS13 gene and inheritance is autosomal recessive .
How do I treat TTP?
Treatment options for TTP refractory to PEX
Corticosteroids. Corticosteroids are used in the acute management of acquired TTP, and should be started upfront together with PEX. Twice-daily PEX. Rituximab. Splenectomy. Cyclosporine. Cyclophosphamide and vincristine. Bortezomib. N-acetylcysteine.
Does TTP cause kidney failure?
TTP happens when too many blood clots that have formed in your blood vessels make it hard for oxygen to reach organs in your body like the kidneys. This can lead to kidney damage and kidney failure. The main sign of TTP is bruising all over the skin that looks like small purple dots.
What is Evans syndrome?
Evans syndrome is a rare disorder in which the body’s immune system produces antibodies that mistakenly destroy red blood cells, platelets and sometimes certain white blood cell known as neutrophils. This leads to abnormally low levels of these blood cells in the body (cytopenia).
What causes Maha?
Possible causes of MAHA include mechanical heart valve, malignant hypertension, vasculitis, adenocarcinoma, preeclampsia/eclampsia, disseminated intravascular coagulation (DIC), thrombotic thrombocytopenic purpura (TTP), and hemolytic-uremic syndrome (HUS)/atypical HUS (see Chapter 20, Disorders of Hemostasis and
Is TTP a disability?
If you are disabled because of Chronic Thrombocytopenia that is so severe it prevents you from working, you may well be entitled to Social Security Disability benefits.
What is the mortality rate of TTP?
The mortality rate of patients with TTP was 90% until the introduction of plasma therapy that increased the survival rate to 70-80%, with minimal or no sequelae. Of the survivors, 30-60% suffer from relapses, often in association with precipitating factors such as infections, surgery, and pregnancy.
How often does TTP occur?
The current rate of occurrence for TTP is about 3.7 cases per million people each year. One estimate places the overall incidence rate at four of 100,000 individuals.
Can you survive TTP?
Before we talk about recovery, we must say that some patients with TTP still die. Most of our patients who died never had a chance for effective treatment; patients who have begun plasma exchange treatment have almost always survived.
Can Covid cause TTP?
Patients with cTTP that become infected with COVID-19 similarly would be at increased risk for an acute TTP episode as a result of the infection and the secondary inflammatory state. Patients with cTTP and COVID-19 infection should be monitored carefully for hemolysis.
Is TTP an emergency?
Thrombotic thrombocytopenic purpura (TTP) is a medical emergency that is almost always fatal if appropriate treatment is not promptly initiated. (Thromb Res. 2020;193:53.) Acquired TTP usually presents as severe microangiopathic hemolytic anemia (MAHA) and thrombocytopenia in a previously healthy individual.



