how to correct auto-peep on ventilator, check these out | How do you fix intrinsic PEEP?
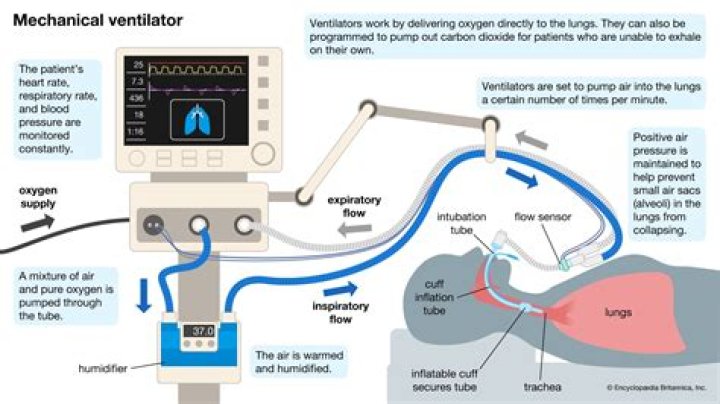
Treating auto-PEEP
Decreasing respiratory rate will increase the time between breaths and decrease the inspiratory to expiratory (I:E) ratio to 1:3 to 1:5.Increasing the inspiratory rate to 60 to 100 L/min will assure fast delivery of air during inspiration, lending more time for exhalation.
How do you fix intrinsic PEEP?
When intrinsic PEEP is diagnosed, the patient should temporarily be released from mechanical ventilation to allow for full expiration. The ventilator can then be adjusted to shorten inspiration by decreasing the set tidal volume, increasing the inspiratory flow rate, or reducing the frequency of respirations.
What causes auto-PEEP on a ventilator?
Auto-PEEP occurs in patients receiving mechanical ventilation in the acute stage of acute respiratory failure when they have excessive minute ventilation, resulting in a relatively short expiratory time. This can be explained by the common phenomenon of a time constant in the exhalation phase.
What methods are used to reduce air trapping and auto-PEEP?
Use of large-diameter endotracheal tubes, bronchodilators, short inspiratory times, long expiratory times, lower respiratory rates and the use of sedatives can be necessary to avoid the dynamic hyperinflation caused by air-trapping.
What mode of ventilation is most effective at avoiding barotrauma?
Whereas low-tidal-volume ventilation has been strongly advocated, plateau pressure may be a more useful parameter to monitor and a better reflection of barotrauma risk in these patients. Low tidal volume is an effective ventilation strategy, but clinicians have been somewhat slow to adopt this approach.
What is intrinsic and extrinsic PEEP?
The two types of PEEP are extrinsic PEEP (PEEP applied by a ventilator) and intrinsic PEEP (PEEP caused by an incomplete exhalation). Pressure that is applied or increased during an inspiration is termed pressure support.
What is the highest PEEP setting on a ventilator?
PEEP of 29 appears to be the highest tolerated PEEP in our patient. We noted an initial rise in blood flow across all cardiac valves followed by a gradual decline. Studies are needed to investigate the immediate effect and long-term impact of PEEP on cardiopulmonary parameters and clinical outcomes.
How do you assess for auto-PEEP?
Although not apparent during normal ventilator operation, the auto-PEEP effect can be detected and quantified by a simple bedside maneuver: expiratory port occlusion at the end of the set exhalation period. The measurement of static and dynamic auto-PEEP differs and depends upon the heterogeneity of the airways.
Which ventilator setting should be changed first for refractory hypoxemia?
Various authors have recommended early (up to 36 h after intubation), high dose prone ventilation (for 12–18 consecutive h/day) as a rescue strategy in patients with severe hypoxemia.
How do you adjust pressure control ventilation?
Set the ventilator mode to assist control, and match the f, FiO2, PEEP, and I:E ratio to the VCV settings. Set the initial inspiratory target pressure at 75% of the difference between Ppeak and PEEP while on VCV. Increase set inspiratory pressure until the desired Vt is obtained.
What is FiO2 on ventilator?
FiO2: Percentage of oxygen in the air mixture that is delivered to the patient. Flow: Speed in liters per minute at which the ventilator delivers breaths.
Can air trapping be reversed?
Your doctor may prescribe a type of medicine called a bronchodilator. It can open up your airways and help reverse the effects of hyperinflated lungs by allowing the trapped air to escape.
What is PIP in ventilation?
The peak inspiratory pressure (PIP) is the highest pressure measured during the respiratory cycle and is a function of both the resistance of the airways and the compliance of the respiratory system.
What does a higher mPaw result in?
Conclusion. HFOV with high level of mPaw increases transpulmonary pressures without improvement in oxygenation.
What is refractory hypoxemia?
There is no standard definition of refractory hypoxemia, and this term usually considered when there is inadequate arterial oxygenation despite optimal levels of inspired oxygen. There is significant heterogeneity in opinions among intensivists regarding the definition, as demonstrated by a recent survey.
Is minute volume and minute ventilation the same?
Minute ventilation (or respiratory minute volume or minute volume) is the volume of gas inhaled (inhaled minute volume) or exhaled (exhaled minute volume) from a person’s lungs per minute. It is an important parameter in respiratory medicine due to its relationship with blood carbon dioxide levels.



