How much does 1 unit of blood raise your hemoglobin?
Introduction: Each unit of packed red blood cells (PRBCs) is expected to raise circulating hemoglobin (HGB) by approximately 1 g/dL.
What is the increase in HGB and HCT after receiving 1 unit of blood?
Whole Blood
One unit of WB should increase the hgb by 1g/dL and hct by 3% in an adult.
How much should hemoglobin go up after transfusion?
Transfusion of one unit of red cells in a non-bleeding patient should increase the patient’s hemoglobin by 1 to 1.5g/dL or hematocrit by 3%. A common practice of some providers is to check the hemoglobin 4 to 8 hours after completion of the transfusion, particularly in a patient with high risk for bleeding.
In general, patients with iron deficient anemia should manifest a response to iron with reticulocytosis in three to seven days, followed by an increase in hemoglobin in 2-4 weeks.
How much does hematocrit increase with 1 unit of blood?
If 1 “unit” of packed red blood cells is approximately 300 mL, this becomes a change of hematocrit of 1.9% +/- 1.2% per “unit” of blood.
When the hemoglobin count is higher than normal, it may be a sign of a health problem. Normal hemoglobin counts are 14 to 17 gm/dL (grams per deciliter) for men and 12 to 15 gm/dL for women.
What is a critical hemoglobin level?
An Hb value less than 5.0 g/dL (50 g/L) can lead to heart failure and death. A value greater than 20 g/dL (200 g/L) can lead to obstruction of the capillaries as a result of hemoconcentration.
What is a critically low hemoglobin level?
Hemoglobin (Hb or Hgb) is a protein in red blood cells that carries oxygen throughout the body. A low hemoglobin count is generally defined as less than 13.5 grams of hemoglobin per deciliter (135 grams per liter) of blood for men and less than 12 grams per deciliter (120 grams per liter) for women.
Grade 1, considered mild anemia, is Hb from 10 g/dL to the lower limit of normal; grade 2 anemia, or moderate anemia, is Hb from 8 to less than 10 g/dL; grade 3, or severe anemia, is below 8 g/dL; grade 4, is life-threatening anemia; grade 5 is death (Table).
What hemoglobin level requires a blood transfusion?
The American Society of Anesthesiologists uses hemoglobin levels of 6 g/dL as the trigger for required transfusion, although more recent data suggest decreased mortality with preanesthetic hemoglobin concentrations of greater than 8 g/dL, particularly in renal transplant patients.
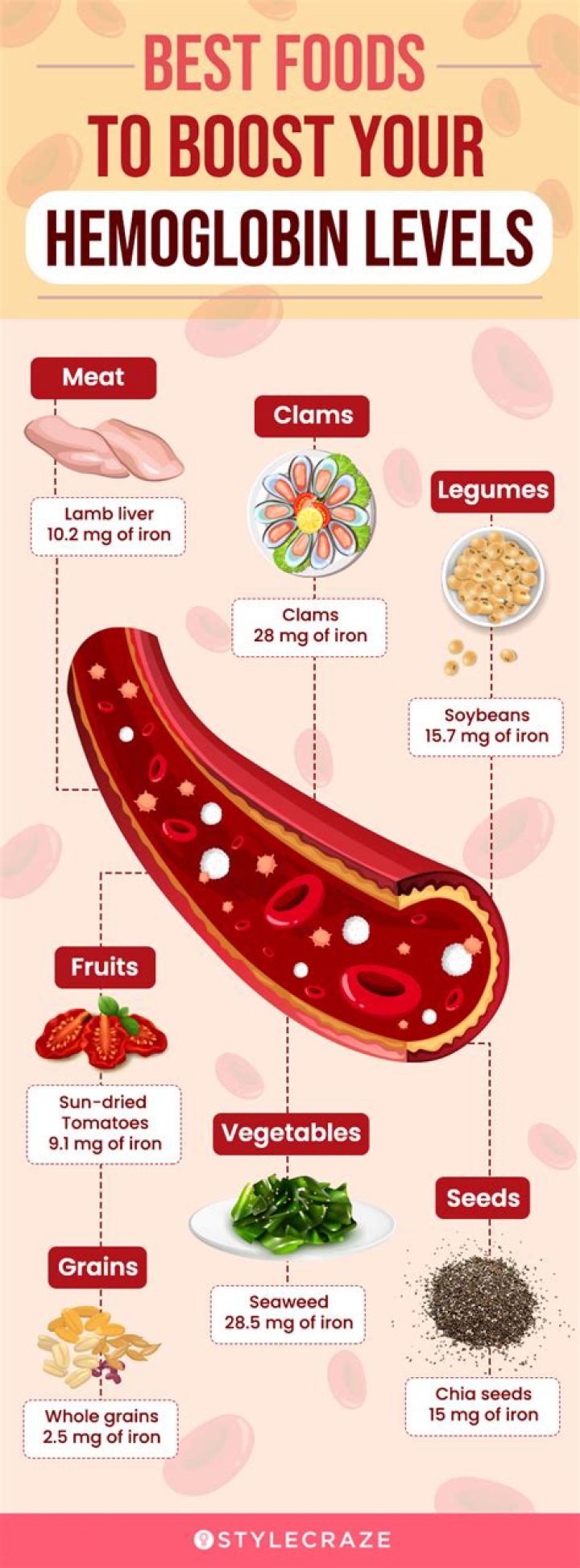
How can I get my hemoglobin up fast?
How to increase hemoglobin
meat and fish.soy products, including tofu and edamame.eggs.dried fruits, such as dates and figs.broccoli.green leafy vegetables, such as kale and spinach.green beans.nuts and seeds.
Is 65 mg of iron a day too much?
At high doses, iron is toxic. For adults and children ages 14 and up, the upper limit — the highest dose that can be taken safely — is 45 mg a day. Children under age 14 should not take more than 40 mg a day.
Many factors can produce hemoglobin fluctuations in the same individual and in a group of individuals. Hemoglobin may decrease as much as 1 gm/dL with bed rest. Changes in fluid balance may affect plasma volume and therefore hemoglobin concentration. Gender and age are responsible for important normal variations.
How much does hemoglobin drop after blood donation?
Frequent blood donation can contribute to anemia because a “whole blood donation” results in a drop of hemoglobin levels by approximately 10 g/L. Healthy donors produce new red blood cells to replace donated cells.
How much does hemoglobin drop with blood loss?
Each unit of blood loss drops the hematocrit by 3 percent points (hemoglobin by 1 mg/dL).
When should you go to the ER for low hemoglobin?
In some cases, iron deficiency anemia can be a serious condition that should be immediately evaluated in an emergency setting. Seek immediate medical care (call 911) if you, or someone you are with, have any of these serious symptoms including: Chest pain or pressure. Difficulty breathing.
In this study, we found that water intake may improve anemia by increasing the hemoglobin index. In the experimental group, the increase in hemoglobin was not significant, although there were significant increases in MCH and MCHC, indicating that water assists hemoglobin synthesis.
What is a healthy hemoglobin level by age?
Normal hemoglobin ranges by age
6 months to 4 years: At or above 11 g/dL. 5-12 years: At or above 11.5 g/dL. 12-15 years: At or above 12 g/dL. Adult male: 13.8 to 17.2 g/dL.
What level of hemoglobin is dangerously high?
Hemoglobin levels greater than 16.5 g/dL (grams per deciliter) in women and greater than 18.5 g/dL in men suggest polycythemia. In terms of hematocrit, a value greater than 48 in women and 52 in men is indicative of polycythemia.



