does horner’s syndrome go away, check these out | How long does Horner’s syndrome last?
There’s no specific treatment for Horner syndrome. Often, Horner syndrome disappears when an underlying medical condition is effectively treated.
How long does Horner’s syndrome last?
If the lesion is not due to any pathological cause, a slow recovery lasting up to several weeks to 4 months can be expected.
Can Horners syndrome be fixed?
There’s no specific treatment for Horner syndrome, but treatment for the underlying cause may restore normal nerve function.
What nerve is damaged in Horner’s syndrome?
In most cases, the physical findings associated with Horner syndrome develop due to an interruption of the sympathetic nerve supply to the eye due to a lesion or growth. The lesion develops somewhere along the path from the eye to the region of the brain that controls the sympathetic nervous system (hypothalamus).
Can Horners syndrome be intermittent?
Intermittent Horner syndrome is uncommon in both the adult and pediatric population. We describe a case of a pediatric patient with an intermittent Horner syndrome. Infrared photography and videography were used to help establish the diagnosis.
Is Horner’s syndrome serious?
A condition that affects the eyes and part of the face, Horner’s syndrome can cause drooping eyelid, irregular pupils and lack of perspiration. Though symptoms themselves aren’t dangerous, they may indicate a more serious health problem.
What are the 3 classic signs of Horner’s syndrome?
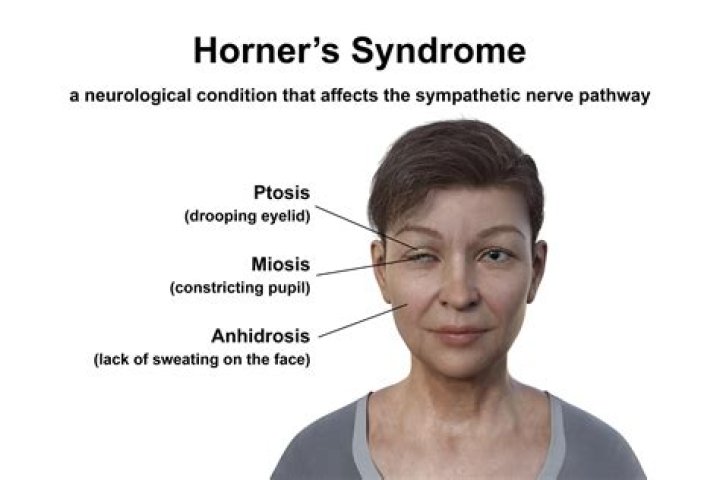
Symptoms of Horner’s syndrome typically include drooping of the upper eyelid ( ptosis ), constriction of the pupil (miosis), sinking of the eyeball into the face, and decreased sweating on the affected side of the face (anhidrosis).
Can ear infection cause Horner’s syndrome?
Horner’s syndrome can result from deep ear infections because the nerves in question pass right through the middle ear (where the eardrum is) and this is where we suspected Nero’s infection was coming from.
Is Horner’s syndrome painful?
De Bray et al. studied the prognosis of 90 cases of isolated Horner syndrome due to internal carotid artery dissection [3]. They found that 91% of cases of Horner syndrome due to internal carotid artery dissection were painful.
When is Horner’s syndrome diagnosed?
Horner’s syndrome is diagnosed clinically by observing ptosis (of upper and lower lids), miosis of the ptotic eye and demonstration of dilation lag in the affected eye, and anhidrosis on the same side as the ptosis and/or mitosis.
Does Horner’s syndrome cause diplopia?
Third order neuron lesions may cause diplopia due to sixth cranial nerve palsy, numbness or pain in the distribution area of ophthalmic and maxillary division of trigeminal nerve ( Vth cranial nerve).
Is Horner’s syndrome ipsilateral or contralateral?
Horner’s syndrome, also known as oculosympathetic paresis, is a combination of symptoms that arises when a group of nerves known as the sympathetic trunk is damaged. The signs and symptoms occur on the same side (ipsilateral) as it is a lesion of the sympathetic trunk.
Why is there anhidrosis in Horner’s syndrome?
Horner syndrome is a rare condition classically presenting with partial ptosis (drooping or falling of the upper eyelid), miosis (constricted pupil), and facial anhidrosis (absence of sweating) due to a disruption in the sympathetic nerve supply.
How common is Horner’s syndrome in babies?
Roughly 5% of cases are congenital, affecting a baby from the moment they are born. There is no specific treatment for Horner syndrome, as the underlying cause must be identified and treated. In some cases, however, the underlying issue may not be treatable.
Can a nerve block cause Horner’s syndrome?
Ipsilateral stellate ganglion block accompanied by interscalene brachial plexus block causes Horner’s syndrome presenting with miosis, ptosis, and anhidrosis. The extent of Horner’s syndrome can be represented by the difference in pupil diameter between bilateral eyes.



