amiodarone moa, check these out | How does amiodarone work on the heart?
After intravenous administration, amiodarone acts to relax smooth muscles that line vascular walls, decreases peripheral vascular resistance (afterload), and increases the cardiac index by a small amount. Administration by this route also decreases cardiac conduction, preventing and treating arrhythmias.
How does amiodarone work on the heart?
It is used to restore normal heart rhythm and maintain a regular, steady heartbeat. Amiodarone is known as an anti-arrhythmic drug. It works by blocking certain electrical signals in the heart that can cause an irregular heartbeat.
Is amiodarone an AV nodal blocker?
In addition to procainamide, newly available parenteral antiarrhythmic agents for treatment of PSVT refractory to vagal maneuvers, adenosine, and AV nodal blocking agents include amiodarone, propafenone, flecainide, and sotalol.
Is amiodarone a calcium channel blocker?
Amiodarone possesses multiple pharmacologic properties, including peripheral and coronary vasodilatation, negative inotropy, and negative chronotropic and dromotropic effects. These properties are shared by the group of drugs termed calcium channel blockers.
Is amiodarone a vasopressor or vasodilator?
Objective: Amiodarone, a class III antiarrhythmic agent, is a potent coronary vasodilator.
How does amiodarone control VT?
After intravenous administration, amiodarone acts to relax smooth muscles that line vascular walls, decreases peripheral vascular resistance (afterload), and increases the cardiac index by a small amount. Administration by this route also decreases cardiac conduction, preventing and treating arrhythmias.
Can amiodarone be given via peripheral line?
Special precautions need to be followed in the use of intravenous amiodarone. To avoid phlebitis, administration through a central venous line is recommended. If the drug is administered through a peripheral line, concentrations should not exceed 2 mg/mL.
Is amiodarone a vasoconstrictor?
We conclude that amiodarone is a powerful systemic and coronary vasodilator. In addition to its present indications in the treatment of angina pectoris and arrhythmias, the drug might be very useful as an afterload-reducing agent.
Is amiodarone a rate or rhythm control?
Amiodarone is more effective than sotalol or propafenone in preventing recurrent atrial fibrillation in patients for whom a rhythm-control strategy is chosen. When long-term amiodarone therapy is used, potential drug toxicity and interactions must be considered.
Is amiodarone a beta-blocker?
Amiodarone is a coronary and peripheral vasodilator (1). Metoprolol is a selective beta1-blocker and exerts a slight vasoconstrictor effect on coronary arteries due to its lack of beta2 stimulation (1).
Does amiodarone block sodium channels?
These findings suggested that amiodarone, like lignocaine, blocks the sodium channel primarily when it is in the inactivated state. Both onset and offset kinetics of the block are very rapid. Such sodium channel blocking characteristics may contribute to its potent antiarrhythmic activity.
Is amiodarone a blood thinner?
“Amiodarone is a common and effective drug used to normalize irregular heart rhythm caused by atrial fibrillation,” Flaker said. “However, because clotting is a complication associated with the condition, an anticoagulant or blood thinner is frequently used to reduce that possibility.
How do you titrate amiodarone drip?
To treat all acute tachyarrhythmias in adults, amiodarone can be given IV 150 mg over 10 minutes, followed by a 1 mg/min infusion for 6 hours, followed by an infusion at 0.5 mg/min. The recommended total dose over 24 hours should not exceed 2.4 grams.
Is amiodarone an Inotrope?
In conclusion, amiodarone exerts acute electrophysiological and inotropic effects in vitro. The class III antiarrhythmic action of amiodarone is linked with positive inotropy.
How do you draw up amiodarone?
To administer a 150 mg bolus: Draw amiodarone 150 mg (3 mL) into a 10 ml syringe. You do not need a filter for the bolus dose. Administer IV direct..
Contraindications include:
Complete heart block without a working pacemaker.Known allergy to amiodarone.Prolonged QT interval.
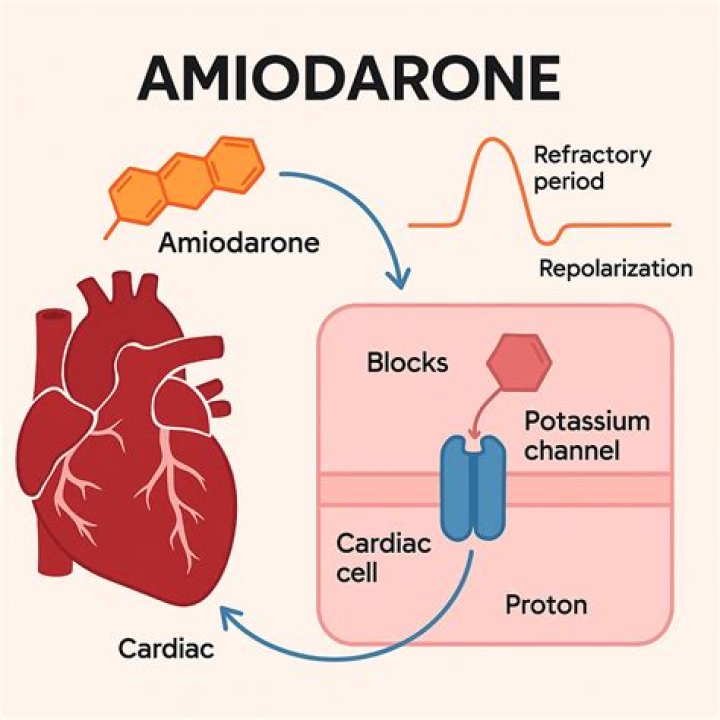
What does amiodarone do to potassium?
Amiodarone has multiple effects on myocardial depolarization and repolarization that make it an extremely effective antiarrhythmic drug. Its primary effect is to block the potassium channels, but it can also block sodium and calcium channels and the beta and alpha adrenergic receptors.
How is amiodarone distributed?
Amiodarone is preferentially distributed in decreasing order in lung, liver, thyroid gland, kidney, heart, adipose tissue, muscle tissue and brain. The metabolite desethylamiodarone exhibited a distribution pattern comparable to the parent drug.



